|
J Shoulder Elb Surg 22(12):1729–1736Īrain AR, Haddad S, Anderson M, Murtaza H, Rosenbaum A (2019) Isolated pediatric transolecranon fracture-dislocation of the elbow managed nonoperatively: a case report and review of literature. Giannicola G, Scacchi M, Sacchetti FM, Cinotti G (2013) Clinical usefulness of proximal ulnar and radial fracture-dislocation comprehensive classification system (PURCCS): prospective study of 39 cases. Rev Chir Orthop Reparatrice Appar Mot 60(7):557–567įoruria AM, Augustin S, Morrey BF, Sanchez-Sotelo J (2013) Heterotopic ossification after surgery for fractures and fracture-dislocations involving the proximal aspect of the radius or ulna. 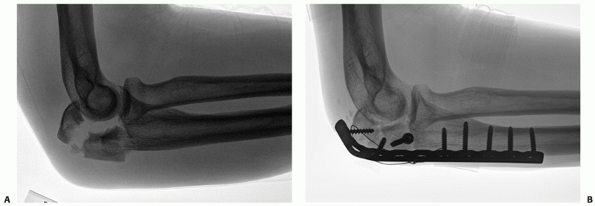
doi: īiga N, Thomine JM (1974) Trans-olecranal dislocations of the elbow. and Beingessner D (2020) Patient outcomes after transolecranon fracture-dislocation. Haller JM, Hulet DA, Hannay W, Cardon J, Tashjian R. In addition, we emphasize that early operation could achieve good clinical outcomes. We recommend open reduction and internal fixation, using either plates or tension-band techniques, depending on the injury pattern. To our knowledge, this is the largest sample size reported to date. 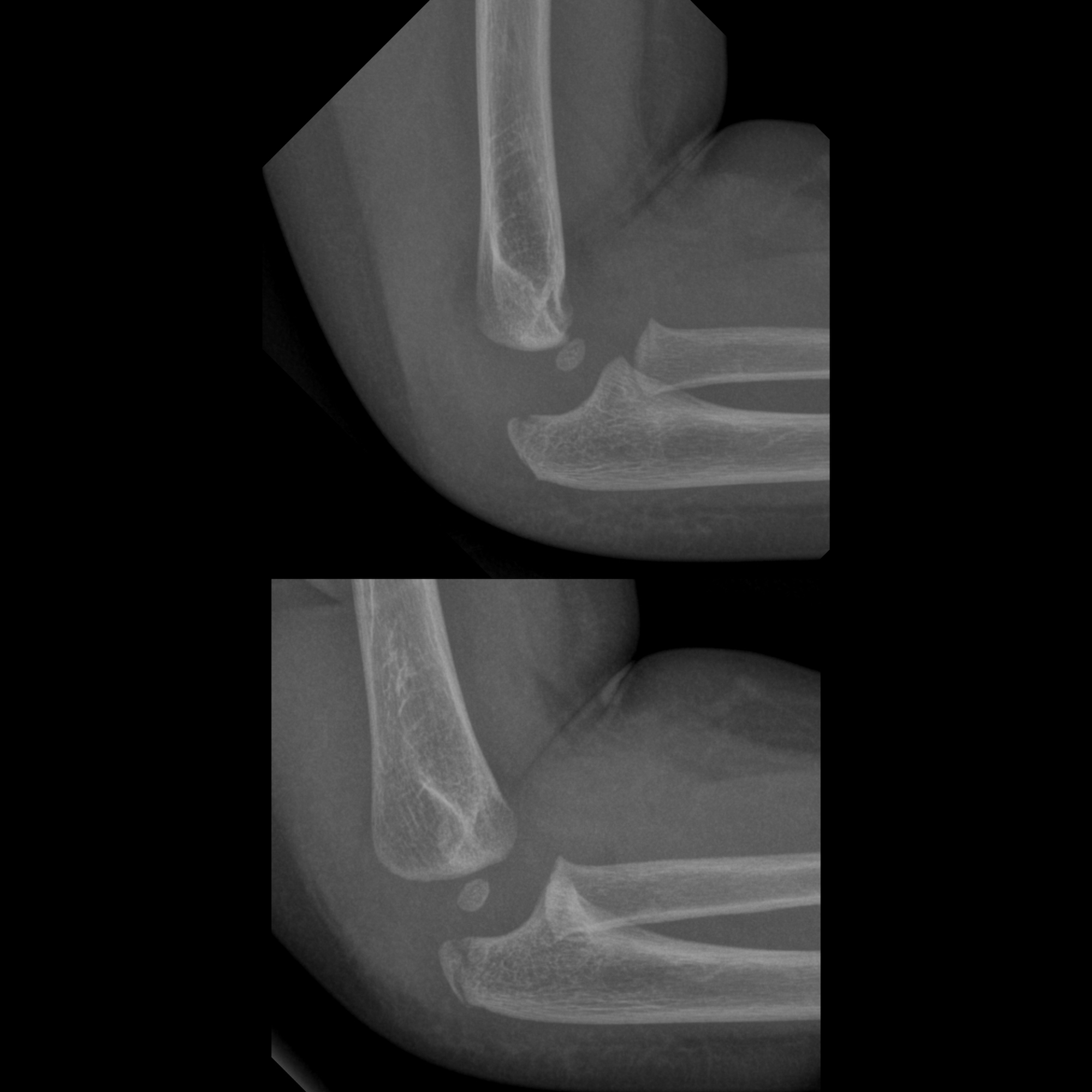
The average operation time was significantly longer in four children sustaining delayed surgery (140 ± 43 min, vs. Four patients were delayed cases, who underwent surgery two weeks after injury. According to the MEPS criteria, the outcomes were excellent in five cases, good in two cases, fair in one case, and poor in three cases. According to Tiemdjo classification, there was one case with type I injury, one case with type II, six cases with type III, and three cases with type IV. The mean age at injury was nine years (range, 4–13 years), and the mean time from injury to surgery was 16.6 days (range, 2–60 days). All injuries were unilateral, and there were nine males and two females. The mean follow-up was 22 months (range, 6–42 months). At the most recent follow-up visit, all patients were evaluated clinically using the Mayo Elbow Performance Score (MEPS). All patients underwent open reduction and internal fixation through a posterior approach. Methodsįrom 2002 to 2019, eleven cases diagnosed with trans-olecranon fracture–dislocation of the elbow were identified, and their medical charts and radiographs were obtained. To provide a clear clinical description and more accurate treatment options, we retrospectively reviewed cases with this kind of injury in our institution. To our knowledge, only 12 cases have been described in children till now and the treatment strategy for this injury in children remains unclear. Fixation by IMN may be indicated for specific situations, but is technically more demanding and has a higher rate of complications.Trans-olecranon fracture–dislocations are rare in children. 
Our findings suggest that open reduction and internal fixation with a DCP remains the best treatment for unstable fractures of the shaft of the humerus. We had to perform secondary surgery on seven patients in the IMN group, but on only one in the DCP group (p = 0.016). In the DCP group three patients developed complications, compared with 13 in the IMN group. Of these six, five occurred after antegrade insertion of an IMN. There was a single case of shoulder impingement in the DCP group and six in the IMN group. There were no significant differences in the function of the shoulder and elbow, as determined by the American Shoulder and Elbow Surgeons’ score, the visual analogue pain score, range of movement, or the time taken to return to normal activity. 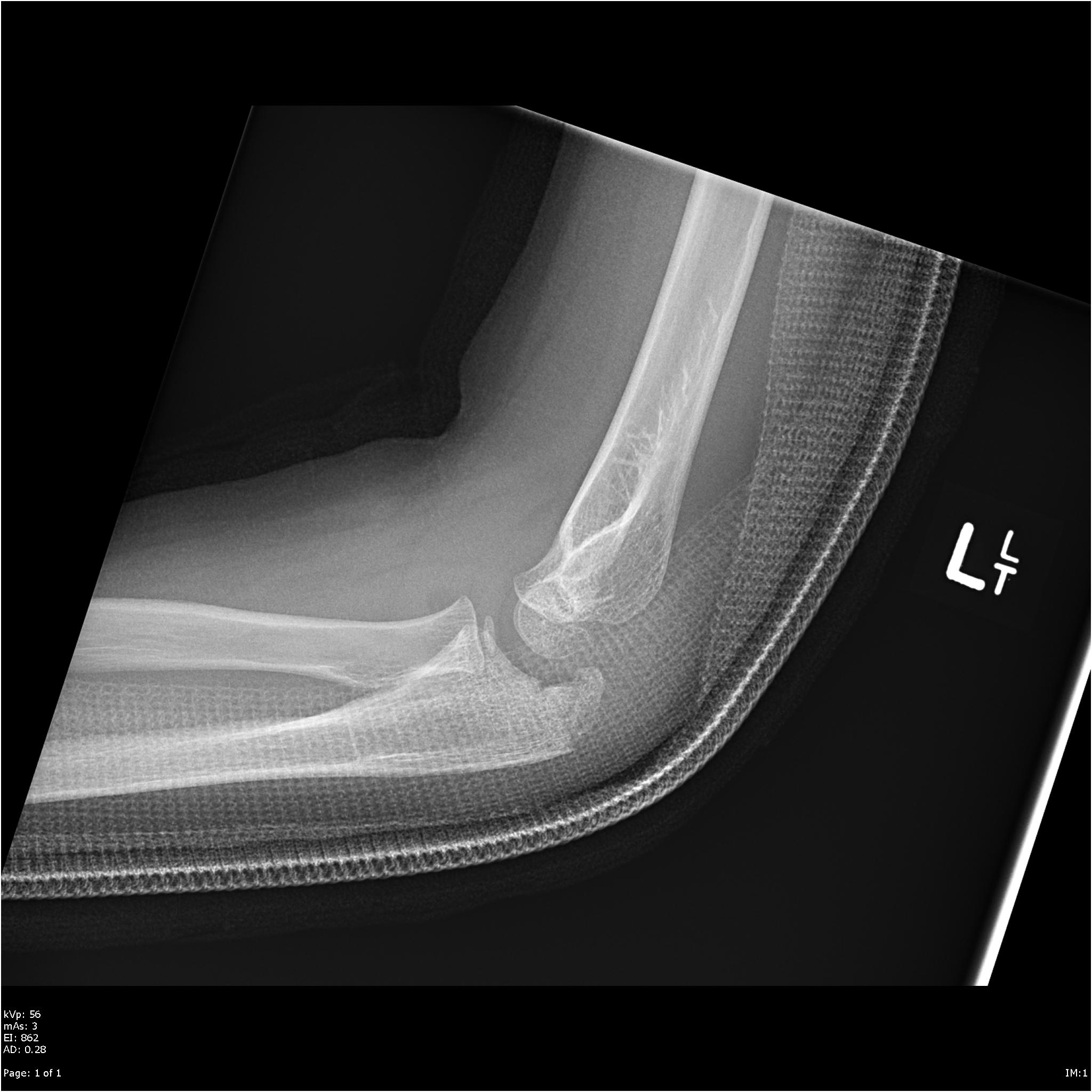
Patients were followed up for a minimum of six months. We randomised prospectively 44 patients with fractures of the shaft of the humerus to open reduction and internal fixation by either an intramedullary nail (IMN) or a dynamic compression plate (DCP).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
